Search
Coming up in 2021 We have a a study to suit every age range in 2021! From babies at just six weeks for the FluBub Study, through to teenagers in

The year that was 2025!
Highlights from the VTG Laboratory in 2025
Conference presentations in 2025
COVID-19 Research Update
Latest news & events at the Wesfarmers Centre of Vaccines & Infectious Diseases.
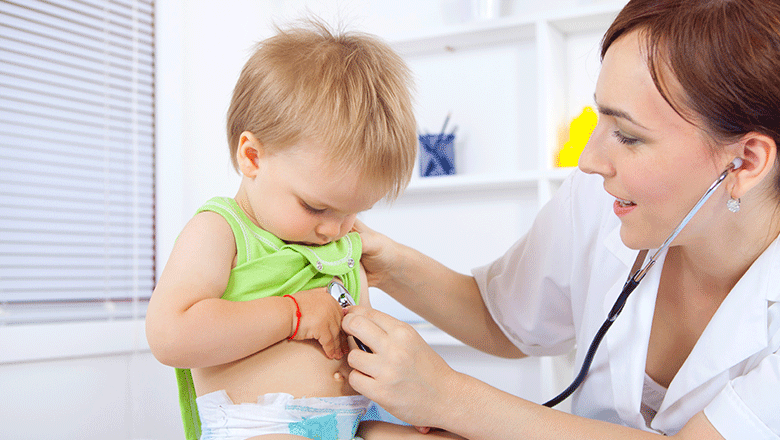
A The Kids Research Institute Australia study designed to gauge community awareness of respiratory syncytial virus (RSV) has found parents and parents-to-be are highly aware of the virus and are open to immunisation to tackle it.

A new National Healthy Skin Guideline has been launched by The Kids Research Institute Australia, to help health care providers identify, diagnose and treat a range of skin conditions experienced by Aboriginal and Torres Strait Islander people in urban and remote areas.

A The Kids Research Institute Australia and Curtin University-led study has found the maternal whooping cough vaccine given to pregnant mothers in the second or third trimester significantly reduced babies’ risk of infection, protecting them at their most vulnerable age.